06 May 2026
New research, published in the Journal of Substance Use in February 2026, shows that peer-to-peer support helps people recover from addiction, particularly for those in early stages of recovery.
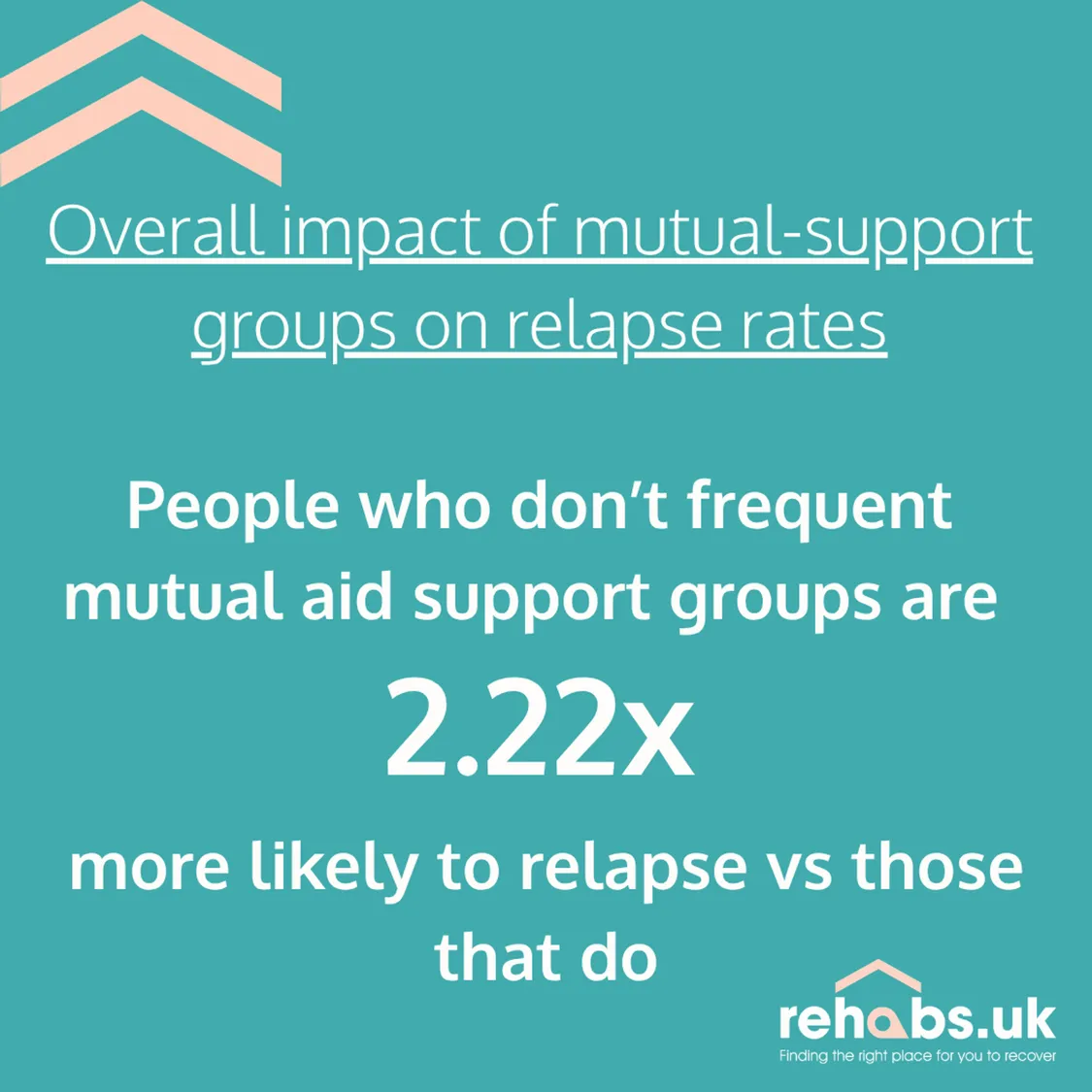
The study, titled ‘Mutual-aid group involvement lowers relapse risk more in early recovery than in later stages’, identified that greater involvement in peer support recovery networks and mutual-aid groups improves early recovery outcomes. It found that people who don’t frequent mutual-aid support groups are more than twice as likely (2.22x) to relapse than people who do.
The research, which surveyed 311 adults who identified as being “in recovery” or “recovered” from problematic drug use for at least 3 months, is part of the growing body of evidence that shows recovery practices like peer-to-peer support are a vital part of addiction treatment.
Recovery is rarely achieved in isolation. Peer-to-peer support has always been important to Rehabs UK, as well as many other treatment organisations and professionals in the addiction field. As Lester Morse, Director of Rehabs UK, explains, the research aligns closely with what recovery professionals have long witnessed in practice:
“Environmental enrichment (EE) is something we observed many decades ago and have been practising with great success for many years. Trying to get that through to mainstream providers has been very difficult, so it’s encouraging to see a growing body of evidence support this.”
In this article, we dive into the findings of the study and explain what addiction treatment providers and policymakers alike should take away from it.
The findings at a glance
- People who don’t frequent mutual-aid support groups are 2.22 times more likely to relapse than those who do.
- The impact of attending mutual-aid groups is highest in early or sustained recovery (up to 5 years).
- For those in recovery for 5 years or more, attending support groups did not significantly affect their chance of relapsing.
Overall impact of mutual support groups on relapse rates
The participants: problematic substances and support group attendance
Participants’ mutual-support group attendance
A total of 86% of the participants reported they had ever attended one or more of the following mutual-aid groups:
- Alcoholics Anonymous: 60%
- Narcotics Anonymous: 63%
- Other 12-step groups: 37%
- Other-peer groups: 37%
- SMART Recovery: 12%
The researchers noted a clear split in participants’ mutual-aid groups engagement. More than one-third (36%) of the participants reported that they had very high involvement in peer support groups, scoring 10 or more points on the 14-point Recovery Group Participation Scale (RGPS) the researchers used. Conversely, almost a quarter of participants (44%) did not frequent mutual-aid groups, or reported low engagement.
Participants’ self-reported problematic substance use
- Alcohol: 67%
- Cocaine (powder): 64%
- Cannabis: 63%
- Amphetamines: 54%
- MDMA: 34%
- Prescription drugs: 34%
- Heroin: 33%
- Crack Cocaine: 31%
Participants could select more than one mutual-aid group and substance.
Research findings
Overall, 22% of the participants reported having experienced a relapse in the time between the two surveys, and 16% said they had experienced problematic use in the 30 days before the last survey.
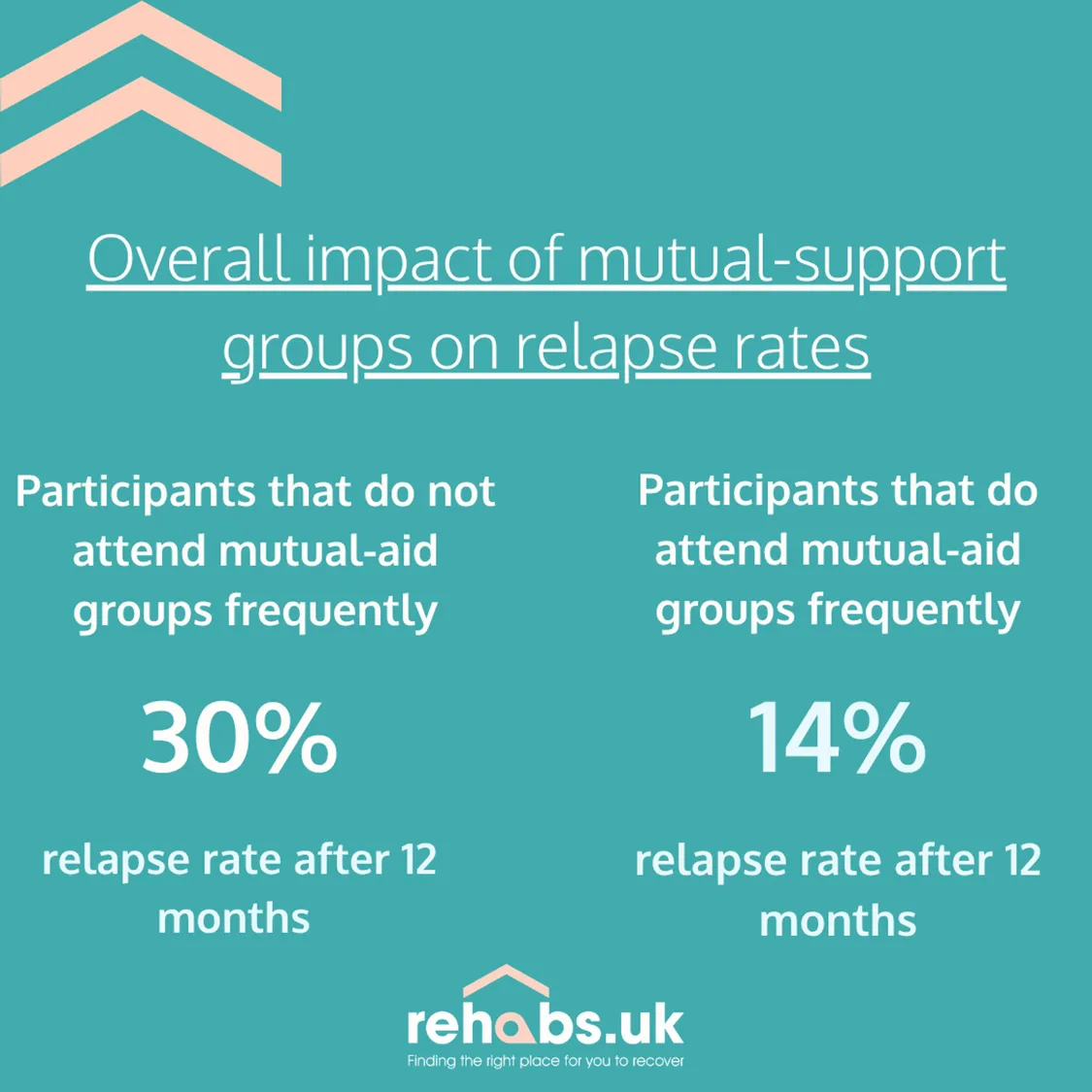
The researchers analysed the likelihood of relapse between those who attend mutual-aid groups regularly and those who don’t. Regardless of recovery stage, 30% of those who don’t attend mutual aid groups regularly reported a relapse, compared to 14% that do.
overall impact of mutual-support groups on relapse rates
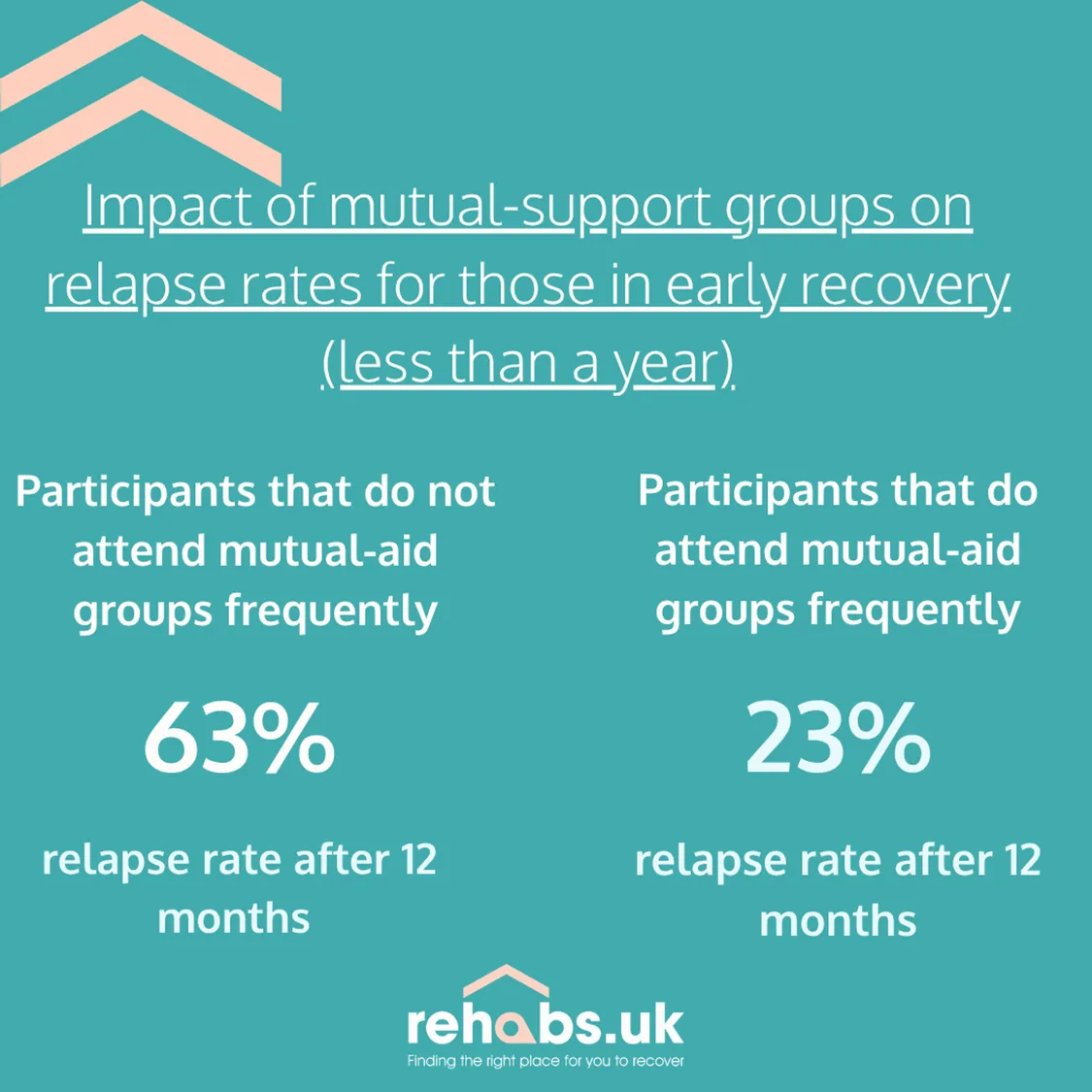
The study found that the impact of mutual-support groups on relapse rates was highest for those who are in early recovery, of less than a year. The results show:
- High engagement in mutual-aid groups correlated with a lower risk of relapse for those in early recovery (less than a year).
- Of those in early recovery, 63% of people who didn’t frequent these support groups reported a relapse.
- In comparison, only 23% of those who engaged regularly in support groups reported a relapse.
- For those in recovery for 1 to 5 years, attending support groups also reduced their risk of relapse.
- Of this group, 37% of those who didn’t frequent support groups reported a relapse.
- Comparatively, only 20% of those who engaged regularly in support groups reported a relapse.
- For those in recovery for 5 years or more, attending support groups did not significantly affect their chance of relapsing.
Impact of mutual-support groups on relapse rates
The research does highlight that continued recovery is not necessarily due to engagement in mutual-support groups alone, and that there are a lot of other factors which might contribute to someone's continued sobriety, such as more established recovery identities and greater personal and social resources.
As mentioned in the research: “It should be acknowledged that this does not mean mutual-aid groups are not beneficial at later stages of recovery, just that other internal or external resources (e.g., social identity, coping, or meaningful activities) likely play a greater role at maintaining recovery at these stages."
What this means for addiction treatment
1. Prioritise peer support integration
The study confirms that higher levels of engagement within the recovery community lead to improved well-being and stronger recovery-oriented social networks.
As mentioned in the study, these groups can: “cultivate crucial mechanisms of change, including instilling a sense of hope, building pro-recovery networks, providing role models, and legitimising the effectiveness of new coping skills.”
When looking specifically at peer-led recovery, Lester Morse notes: “These communities create a safe space. They provide social and psychological resources, which can include accountability, emotional support and a sense of belonging. This resonates again when examining the study's results. Those who didn’t partake in peer-led recovery groups such as AA or NA scored higher at baseline and had a higher chance of relapsing after 12 months.”
The study’s findings confirm that addiction treatment plans and policies must actively integrate peer-led recovery communities.
2. Target the fragile early recovery window
The study highlights that the early recovery stage is particularly fragile as those who are in their first year of recovery face a higher risk of relapse. It also notes that people in the early stages of recovery require greater external support, with recovery evolving into a “self-sustaining phase” after 3 to 5 years.
Mutual-aid groups, where peers support each other, give people the resources to build and sustain their recovery. It has also been shown to be a cost-effective and evidence-based intervention in addiction treatment (Kelly et al.)
Morse adds: “At Rehabs UK, we recognise that early recovery is one of the most challenging stages in the recovery journey. In this stage, individuals are starting to make the transition away from substance use and trying to put into practice new coping strategies they’ve learned, as well as navigate a range of different social environments.”
Addiction treatment providers must recognise this period as high risk, and encourage involvement in mutual-aid groups.
3. Invest in recovery communities
Lived experience is the key to early recovery. This is why peer support is so important and can be extremely powerful, as it offers something that addiction services cannot on their own.
Morse posits that the concept links to the idea of environment enrichment, which means a recovery environment for individuals where supportive relationships and healthy behaviours are used to reinforce positive change.
“The simple way it was explained to me many years ago was that a sick brain cannot cure a sick brain. If you have people in the peer group who understand how to stay sober and you are willing to trust and listen to them, that environment holds the brain in recovery.”
At Rehabs UK, we express how important structured recovery communities are, including mutual-aid groups such as Alcoholics Anonymous and others linked to addiction. Recovery cafes are also another type of community space that offers a safe, supportive, and non-judgmental environment for individuals recovering from addiction. Staffed by trained volunteers or professionals, often with lived experience, they provide social connection, activities, and recovery resources.
Being around others who truly understand it can make it slightly easier to build and develop healthier thought patterns over time.
Morse explains: “When recovery is strong in that environment, the brain automatically starts to recover and develop new ideas. In AA, they say ‘keep coming back’. Over time, the neural pathways redevelop the capacity to choose to stay sober.”
In other words, recovery communities can help individuals retrain the brain through repeated exposure to supportive behaviours and recovery-focused thinking.
About the study
Participants were from the Netherlands, Belgium, and the UK, and the research was part of a multi-country cohort study by Best et al, titled “REC-PATH, Recovery pathways and societal responses in the UK, Netherlands and Belgium.”
The first survey was conducted between September 2018 and January 2019. A total of 367 adult participants completed this baseline “Life in Recovery” survey and agreed to be contacted for the follow-up. 311 participants completed this follow-up survey 12 months later, between September 2019 and January 2020.
Besides demographic and short qualitative questions, the survey included scales that were designed to draw conclusions about the role that mutual-aid groups play in recovery, including:
- Recovery stage: in the baseline survey, participants were asked how long they had been in recovery.
- Early recovery: <1 year
- Sustained recovery: 1-5 years
- Stable recovery: >5 years
- Recovery Group Participation Scale (RGPS): designed to measure the level of the participant’s involvement in mutual-aid groups.
- Commitment to Sobriety Scale (CSS): designed to measure how committed the participants were to staying abstinent.
- Relapse: in the follow-up survey, participants were asked whether they had relapsed in the past 12 months.
- Problematic use: in the follow-up survey, participants were asked whether they used a range of substances problematically.
The researchers analysed the differences between the baseline survey and the follow-up survey to assess the relationship between mutual-aid group involvement and risk of relapse.
Limitations of the study
The limitations of this study are the definition of “problematic usage”, which means that the participants could have a varied opinion on what they interpret that to be. The study was also self-selected, which means the participants volunteered themselves; this may not have created an accurate, balanced sample. The difference between SMART recovery groups and 12-step groups was also not possible to measure for comparison, as many participants attended both.
“Together we recover, divided we die alone”
For anyone in recovery, the overall message from the research study and Rehabs UK professionals is clear: connection matters.
Peer-support and mutual-aid groups provide guidance, community and understanding during an extremely vulnerable and sometimes scary period of recovery.
As Morse puts it: “Addiction thrives in isolation. We all need each other. The best help you can get is being surrounded by peers. Together we recover – divided we die alone.”
The latest research reinforces this perspective. It suggests that peer support can significantly improve recovery outcomes and continues to strengthen Rehab UK's long-standing perspective that peer-to-peer recovery support should be available to everyone and anyone who needs it.
If you or anyone you know is struggling with addiction, please do not hesitate to contact our Treatment Advisors today.
